


If you or someone in your family has vitiligo, you already know the particular anxiety it creates. Not because it's painful or physically harmful — but because it's visible, unpredictable, and surrounded by so much misinformation. Patients come to Sood Aesthetics in Bangalore with years of confusion behind them: "Is it contagious?" (It isn't.) "Will it spread everywhere?" (Not necessarily.) "Can it be cured?" (The honest answer is nuanced — and that's exactly what we'll cover here.)
Vitiligo gets over 8,000 monthly searches in India, yet most people still don't fully understand what it is or what options exist. Let's change that.
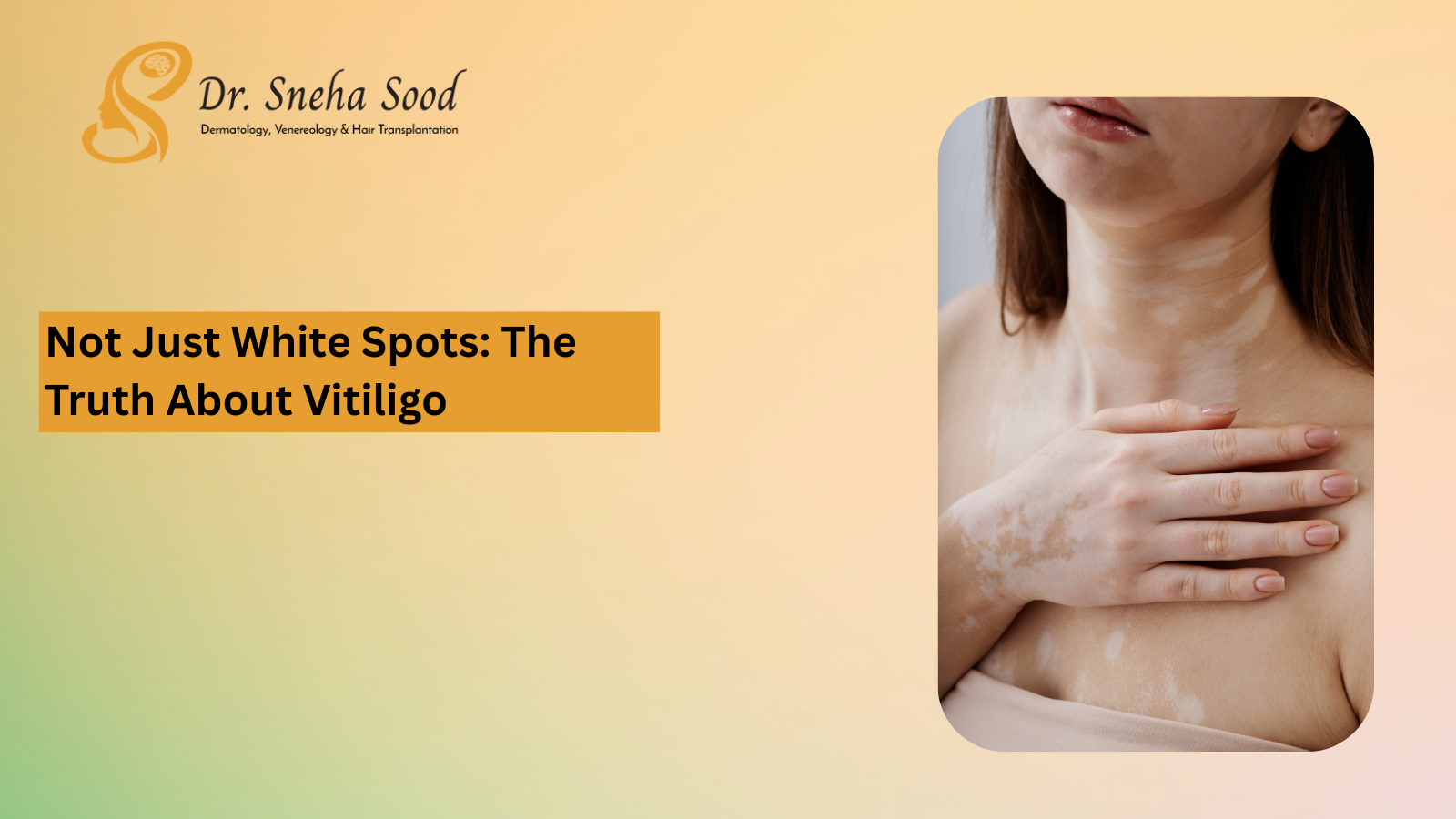
Vitiligo is an autoimmune condition in which the immune system mistakenly attacks and destroys melanocytes — the cells responsible for producing skin pigment (melanin). The result is patches of skin that lose their colour, appearing white or pale pink. It can affect any part of the body and, in some cases, the hair and mucous membranes too.
It is not caused by poor hygiene, diet alone, or sun exposure. It is not contagious. And it is not simply a cosmetic issue — it carries a real psychological and social burden that deserves to be taken seriously.
The exact trigger varies between individuals, but several factors are well-established:
In India's population, which predominantly has deeper skin tones (Fitzpatrick types IV–VI), vitiligo patches are highly visible due to the contrast between affected and unaffected skin. Bangalore's year-round sun exposure also means unprotected vitiligo patches sunburn easily, which can cause additional discomfort and trigger further spread at those sites.
Treatment aims to stop further spread and restore pigmentation where possible. Dr. Sneha Sood at Sood Aesthetics tailors management to the patient's vitiligo type, extent, and activity:
Re-pigmentation is possible and has been demonstrated in numerous clinical trials, particularly for facial and trunk patches treated with phototherapy or excimer laser. Results vary by location (facial vitiligo responds better than hands and feet), patient age, and disease duration. The earlier treatment begins, the better the outcomes generally are.
At the first appearance of a white patch — don't wait to see if it spreads. Early active vitiligo is more responsive to treatment than long-established, widespread disease. Dr. Sneha Sood conducts a Wood's lamp examination and full clinical assessment to stage the disease and begin appropriate management.
Vitiligo is not untreatable, and you don't have to simply accept spreading white patches. With the right diagnosis, appropriate systemic and topical treatment, and consistent sun protection, many patients achieve meaningful re-pigmentation and stability. The key is early, expert-guided intervention — not waiting and hoping it resolves on its own.
Genetic factors do play a role — having a first-degree relative with vitiligo increases your risk. However, it is not a certainty, and many patients have no family history.
Complete cure in the traditional sense is not guaranteed, but significant re-pigmentation and long-term stability are achievable with treatment. Many patients see dramatic improvement.
Yes — there is a well-established association between vitiligo and autoimmune thyroid conditions (Hashimoto's thyroiditis, Graves' disease). Thyroid function tests are recommended at diagnosis.
Not necessarily. Some patients have stable vitiligo that doesn't spread for years. Others experience active phases of spreading followed by periods of stability. Treatment aims to arrest active spreading.
Yes, and this is taken seriously. The visible nature of vitiligo on Indian skin tones creates significant psychological burden for many patients. Support, counselling, and camouflage guidance are all part of comprehensive management.